Due December 31, 2023
A Gag Clause Prohibition Compliance Attestation (GCPCA) is an attestation of compliance with Internal Revenue Code (Code) section 9824, Employee Retirement Income Security Act (ERISA) section 724, and Public Health Service (PHS) Act section 2799A-9, as added by section 201 of Title II (Transparency) of Division BB of the Consolidated Appropriations Act of 2021.
Passage and implementation of the Consolidated Appropriations Act (CAA) of 2021 creates new opportunities for health plans by mandating access to critically important insights into the prices you are paying for your member health care services; details you have most likely been unable to obtain previously from medical and pharmacy carriers due to existing gag clauses that precluded access to data. The removal of gag clauses from medical and pharmacy contracts is your responsibility and should include a thorough review of BAA’s and NDA’s you have in place with medical and pharmacy carriers.
Although the CAA-2021 amends ERISA laws, public sector employers must also attest that all gag clauses are removed from contracts to give unfettered access to data to make more informed healthcare decisions.
Things to know:
CAA compliance jurisdiction and enforcement rests with three government agencies:
- Department of Labor (DOL)
- Internal Revenue Service (IRS)
- Health and Human Services (HHS)
CAA created two key actions:
- Healthcare pricing transparency and access to health plan data (all health plans)
- Fiduciary process mandate for Health Plan Sponsors (ERISA health plans)
What is a Gag Clause:
A gag clause is a provision in a health plan legal agreement (ASO, TPA, PBM, Network) that restricts access to data and sharing of unit cost and provider quality information. Gag clauses prohibit specific analysis among data sets. These clauses do not include the words ‘gag clause’ and are interwoven in the legal agreements Health Plan Sponsors sign with third parties who administer elements of their health plan.
What is the Regulation:
The Consolidated Appropriations Act of 2021 in Section 201 “INCREASING TRANSPARENCY BY REMOVING GAG CLAUSES ON PRICE AND QUALITY INFORMATION,” prohibits Health Plan
Sponsors from entering into agreements with healthcare providers, third-party administrators, and other service providers, which would directly or indirectly restrict the plan sponsor from accessing, owning, and benchmarking certain cost and quality health plan data.
Said differently, Health Plan Fiduciaries cannot be party to a contract that restricts their ability to perform their fiduciary duties of monitoring and assessing plan vendor performance and assessing unit cost for reasonableness.
Why is it necessary:
Most Employer and Multi-Employer Health Plan legal agreements today from Insurance Carriers, Third Party Administrators (TPAs), Provider Networks, Pharmacy Benefit Managers (PBMs) and other third-party vendors contain gag clauses that restrict access and visibility to many hidden cost and intermediary fees that are not disclosed to plan sponsors. This opaque environment has been fertile ground for excess cost layers and bloated unit cost layers to multiply which make healthcare unaffordable for participants. The endgame for CAA is to not allow this opaque environment to happen anymore.
How does this benefit the Plan Sponsors:
When Gag Clauses are removed, Plan Sponsors gain access to all unit cost information with fully transparent agreements and data access. An activated fiduciary process that leverages this data will expose unnecessary cost, so employers can remove it, then pay less for healthcare.
Common Gag Clauses prevent:
- Benchmarking and co-mingling from multiple companies.
- Using data to develop or use any type of pricing transparency tool.
- Using claims data to create any type of healthcare comparison database.
- Using claims data to do cross-carrier comparisons.
- Using claims data to shop carrier services.
- Using claims data to contract with business coalitions, ACO’s or Centers of Excellence.
- Using data to steer patients between providers of the same service, type, or category.
- Performing certain types of analytical procedures on claims data.
- Maintaining the employer’s own claims data history or sharing claims data with a new carrier.
- Carriers from sharing relating to mental health or substance abuse data.
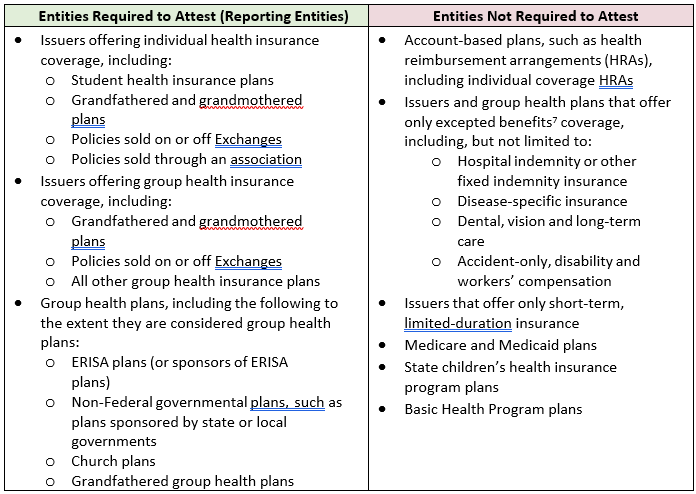
What you need to do:
To submit your health plan’s attestations, go to:
Once on the site, you will see the following resources to assist you. The bottom link “Enter Webform Now for a GCPCA” will take you to the required form.

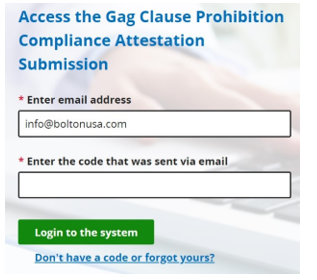
Note when you first login, you need to enter your email address, and then click on “Don’t have a code or forgot yours” – it may take up to 10 minutes to receive your code. Save your code for future use of the site.
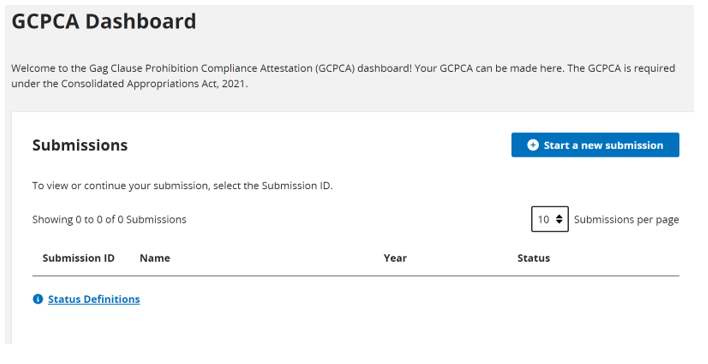
The submission page should look like the following screenshot. After you’ve made your final submission, CMS recommends returning to your dashboard to confirm the “status,” shown on the bottom right side of the following screenshot, indicates it was submitted.
In the meantime, plan sponsors can take several concrete steps to tackle their requirement to strip gag clauses out of their service agreements:
- Gather all service agreements and vendor contracts that concern health care price and quality, including your PBM contract.
- "Test" out the CMS website early...don't wait until the last second.
- Enlist the help of trusted, independent third-parties like Bolton that are well-versed in reviewing benefit plan service provider contracts for gag clauses.
- Identify impermissible gag clauses in service contracts.
- Negotiate the removal of gag clauses from all service provider contracts, confidentiality agreements, and NDAs. Pay special attention when entering new contractual agreements after a marketing or procurement process. Add language to clearly define expectations around gag clauses.
- Negotiate contract amendments to ensure vendor cooperation in meeting your fiduciary obligations, especially those related to the CAA’s gag clause provisions.




